Irritable Bowel Syndrome
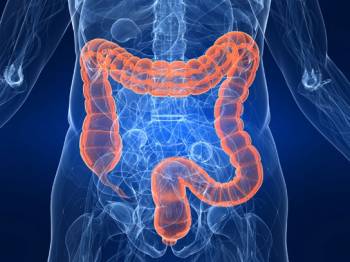 Irritable Bowel Syndrome (IBS), is a common disorder, affecting up to as many as 10 - 15% of people. Whilst most people experience digestive problems once in a while, people with IBS get frequent, recurrent symptoms, which can significantly affect their quality of life.
Irritable Bowel Syndrome (IBS), is a common disorder, affecting up to as many as 10 - 15% of people. Whilst most people experience digestive problems once in a while, people with IBS get frequent, recurrent symptoms, which can significantly affect their quality of life.
In Singapore, up to about 10% of people suffer from Irritable Bowel Syndrome(IBS). People with IBS suffer from recurrent bouts of abdominal pain associated with diarrhoea, constipation, or a combination of the two. Either way, sufferers of IBS end up with frequent doctor visits, limitations in their food choices and reduced productivity at work.
IBS is a "functional disorder" meaning that patients with IBS have no signs of inflammed or damaged tissue or structural abnormalities in the digestive tract.
WHAT ARE THE SYMPTOMS?
The symptoms and severity of IBS can vary from person to person, generally being more common in women. In women, their symptoms of IBS may be made worse around the time of menstruation. Classic IBS symptoms are abdominal pain, associated with constipation , diarrhoea or a combination of both.
In general, IBS symptoms may be classified as being “gut-related” and “non-gut-related”.
“GUT-RELATED" SYMPTOMS
1. Abdominal Pain:
The pain of IBS may range from being a dull ache or discomfort, to severe crampy pains. The pain may be relieved after bowel movements.
2. Changes in Bowel Function:
IBS is classified according to whether it is (i) Constipation-predominant (IBS-C), (ii) Diarrhoea-predominant (IBS-D) or (iii) Mixed (IBS-A).
3. Bloatedness, “wind” or churning in the abdomen
4. A feeling of “urgency”, that you may not make it to the toilet in time.
5. A feeling of “incomplete evacuation”, like there is always still something left behind after bowel movements.
6. Mucous in the stools
“NON-GUT-RELATED" SYMPTOMS
1. Backache
2. Fatigue
3. Discomfort during sexual intercourse
4. Headaches
ASSOCIATED CONDITIONS
IBS is also associated with a higher incidence of depression, anxiety, fibromyalgia and chronic fatigue syndrome.
"RED FLAG" FEATURES
There are certain symptoms or signs which suggest more serious conditions. The presence of any of these features would make the diagnosis of IBS unlikely, thus warranting further investigation.
These so called "RED FLAG" features include:
• Unexplained weight loss
• Fever
• Blood in stools (visible or occult)
• Pain that interferes with sleep
• Diarrhoea that interferes with sleep
• Abnormal physical examination
WHAT CAUSES IBS?
IBS is a "functional disease" and the actual cause of IBS is unknown, however, whatever the cause, it can be put down to the gastrointestinal tract functioning differently in people with IBS.
There are 2 main theories:
1. Abnormal Intestinal Movement
The smooth muscles of the intestines normally undergo alternating contraction and relaxation (peristalsis) to push food down the tract. In diarrhoea due to IBS, the food passes through the intestinal tract too quickly, whilst in the constipation-predominant type of IBS, food passes through too slowly. The pain may coincide with these abnormal contractions.
2. Visceral Hypersensitivity
People with IBS appear to be more “aware” and “sensitive” to normal peristaltic movements of the gut. Whilst most people do not perceive normal gut movements, people with IBS may perceive these movements as pain.
Possible triggers of IBS may include:
• stress
• a bout of gastroenteritis (known as post-infective IBS)
• food intolerance (rather than food allergies)
• alcohol
• caffeine
• smoking
• certain types of medication
HOW IS IBS DIAGNOSED?
 There is no simple test for IBS. Diagnosis is made based on symptoms and excluding other possible causes for your symptoms. Therefore, your doctor will ask you questions about your symptoms and then perform an examination of your abdomen and/or your back passage (a rectal examination). Depending on your risk factors, some simple tests may be done. You may also need a referral to a specialist for further tests.
There is no simple test for IBS. Diagnosis is made based on symptoms and excluding other possible causes for your symptoms. Therefore, your doctor will ask you questions about your symptoms and then perform an examination of your abdomen and/or your back passage (a rectal examination). Depending on your risk factors, some simple tests may be done. You may also need a referral to a specialist for further tests.
Rome II Criteria:
The Rome II criteria (more recently the Rome III criteria has been issued, incorporating some changes to the Rome II criteria) is used to help physicians diagnose IBS. It specifies that people with IBS should have suffered from abdominal pain for 12 consecutive week during the past 12 months. The pain should have 2 of the following 3 features:
1. It is relieved by having a bowel movement.
2. It is associated with a change in stool frequency.
3. It is associated with a change in the appearance of stools.
Other features that cumulatively support the diagnosis of IBS include:
• Abnormal stool frequency (normal stool frequency being defined as having between 3 bowel movements per day to 3 bowel movements per week)
• Abnormal stool form (hard or loose/watery stools)
• Abnormal stool passage (urgency, excessive straining, or feeling of incomplete evacuation)
• Feeling of abdominal bloating/distention.
Tests performed may include:
• Full Blood Count (FBC) with Electrocyte Sedimentation Rate (ESR):
The FBC is done to check for anemia or signs of infection. A raised ESR level indicates likely inflammation.
• CEA levels:
CEA is a marker used for colon cancer. In patients with colon cancer, CEA levels are typically significantly raised. There are, however, also other causes of raised CEA levels.
• Stool analysis:
Stools for faecal occult blood are done as a screen for colon cancer. In the diarrhoea-predominant type of IBS, stools may be sent for culture to check for bacteria, eggs of worms, cysts or parasites.
• Colonoscopy:
Patients above 50 years of age, those at risk of colon cancer, or those with alarm bell symptoms or signs, should have a colonoscopy done by a specialist.
• Thyroid Function Tests:
Abnormally high or low levels of thyroid hormones can cause diarrhoea or constipation respectively.
WHAT IS THE TREATMENT?
The lack of understanding of the physiological mechanisms causing IBS prevent doctors from having treatment targeting these mechanisms. Treatment is instead directed at the symptoms of IBS as well as avoiding known triggers of the condition.
Management of IBS would include:
• Lifestyle Modifications
• Dietary Changes
• Taking Medication
• Reducing Stress Levels
• Complementary or Alternative Treatments
Try each strategy in turn or in combination. Over time, you will learn to recognize which works best for you.
LIFESTYLE MODIFICATIONS
You will probably have to experiment with making changes in the following aspects to see if your symptoms of IBS improve. Lifestyle changes may include:
• Stopping intake of caffeine
• Giving up smoking
• Systemic elimination of food groups in your diet (to be discussed with your doctor)
• De-stressing your life
• Regular exercise
• Allowing time for regular defaecation
DIET CHANGES
Avoidance of foods to which one may be intolerant. This will take much trial and error to figure out, because what may work for one person, may do nothing for another. The importance of eating a healthy and balanced diet cannot be overstated.
Increased soluble fibre intake is beneficial in the constipation-predominant type of IBS. Because fibre adds to the bulk of stools and increases transit through the gastrointestinal tract, it is easy to understand how it can help improve constipation-predominant IBS, whilst making diarrhoea-predominant IBS potentially worse. The best solution is to judge for yourself whether fibre helps or worsens your IBS symptoms and base any dietary changes on this.
Our gut contains friendly gut microflora which are essential for the health of the gut. Using these friendly gut microflora (probiotics) may be beneficial in the treatment of IBS, although more studies are required to determine the efficacy of the different strains of beneficial bacteria, before firm recommendations can be made on their use.
MEDICATION
Drugs are prescribed to treat the predominant symptoms of IBS. For instance, laxatives are used to treat constipation-predominant IBS and antidiarrheals are used to treat diarrhoea-predominant IBS. Anti-spasmodic agents are used to help with the cramps associated with IBS.
Low dose antidepressants have also been shown to be effective in managing IBS.
DE-STRESSING YOUR LIFE
Constant worry about work, family, finances and relationships etc can all significantly worsen the symptoms of IBS. Even the mere worry of IBS helps to fuel the self-perpetuating circle of stress. Here are some things you can do to reduce your stress level:
• Regular exercise
• Ensure you get sufficient good quality sleep
• Meditation and relaxation therapy
• Psychotherapy and Cognitive Behaviour Therapy
IBS is something that will likely affect you on and off for the rest of your life. If it is properly managed, it should not end up dictating what you can or cannot do.
COMMON MYTHS ABOUT IBS:
FOOD ALLERGY VS FOOD INTOLERANCE
What is the difference?
Food allergies are triggered by the body's immune system. If you consume a food to which you are allergic, an immune cascade reaction is triggered. This can result in rash, itching, swelling, breathing difficulties, collapse and even death. Foods that may cause allergic reactions include: shellfish (prawns, crabs, lobster, crayfish), peanuts, alcohol and eggs.
Food intolerance, on the other hand, does not involve the immune system and is thus not an allergy. It occurs when something in a food irritates a person's digestive system or when a person is unable to properly break down the food. Food intolerance is much more common than food allergies and most food intolerances involve diary products, wheat, potatoes, corn and coffee. Symptoms tend to be more localized to the gastrointestinal tract, and they include abdominal pain, diarrhoea, vomiting, palpitations and occasionally rash and flushing.
Skin prick tests used to diagnose food allergies cannot be used in the diagnosis of food intolerance. Unfortunately, there is no simple way for evaluating this condition. The only way is through systematic elimination of possible foods in the diet. This is, however, not as easy as it sounds, because few people are intolerant to just one food type.
Types of food intolerances include:
• lactose intolerance (inability to digest diary products)
• gluten intolerance (inability to digest gluten, the protein found in wheat and certain grains)
• intolerance to certain additives and preservatives in foods (eg. Monosodium glutamate, food colouring)
If you suspect that you may be food intolerant, you should discuss with your doctor how to eliminate it from your diet to see if it makes any difference to your symptoms. Keeping a “Food Diary” in which you chart your diet and symptoms would be useful.
Further Reading
The article above is meant to provide general information and does not replace a doctor's consultation.
Please see your doctor for professional advice.
