COLORECTAL CANCER : A CLEAR AND PRESENT DANGER
Singapore and Malaysia have one of the highest numbers of colorectal cancers in Asia. Not unlike that observed in Caucasian populations, more than 75 percent of colon cancers affect the left sided colon (splenic flexure, descending, sigmoid and rectum) with the rest occurring in the caecum, ascending, hepatic flexure and transverse colon.
RISK FACTORS
Lifestyle
While smoking, lack of exercise and alcohol intake show tenuous links with colon cancer, increase dietary intake of fat and animal protein have demonstrated more consistent associations with Increase risk of colorectal cancer. Fibre and calcium ingestion seem to lower the risks. The evidence is by no means conclusive although various hypotheses have emerged to explain the possible mechanisms.
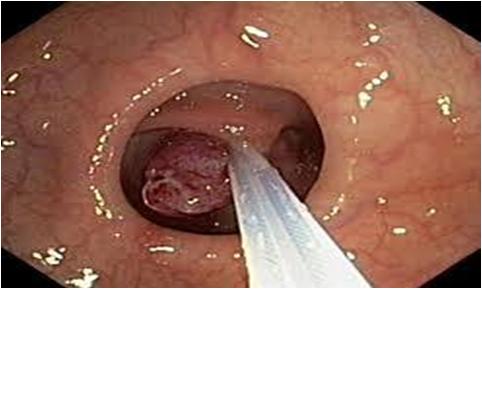 Colonic Polyps
Colonic Polyps
Between 70 and 90 percent of colorectal cancers arise from polyps. Larger (10 mm or more) polyps have a greater potential for malignancy while small polyps (5 mm or less in diameter) have a negligible malignant potential.
The average time from onset of a polyp to onset of cancer, termed the “dwell time,” is 10 to 15 years. This dwell time appears to vary with the location of the cancer - longer in the distal colon than in the proximal colon.
Genetic Factors
A family history of colorectal cancer or polyps increases the risk of colorectal cancer. In general, closer familial relationships to affected relatives, younger age of affected relatives and larger numbers of affected relatives increase this risk. A family history of having a first degree relative (parent or sibling) develop colorectal cancer before the age of 60 or having at least two first degree relatives with these conditions imparts an increased risk for colorectal cancer.
Familial adenomatous polyposis is a genetic condition in which hundreds of polyps develop in the colon and other parts of the gastrointestinal tract, beginning early in life. Persons with familial adenomatous polyposis have an almost 100 percent chance of developing colon cancer by the age of 40.
In hereditary nonpolyposis colon cancer, a strongly inherited tendency for colon cancer is associated with far fewer polyps than occur in familial adenomatous polyposis. Up to 6 percent of colon cancers occur in association with this disorder, which is also called Lynch syndrome. Invariably, about 75 percent of patients with the Lynch syndrome will have colon cancer by the age of 65 years.
EARLY DIAGNOSIS
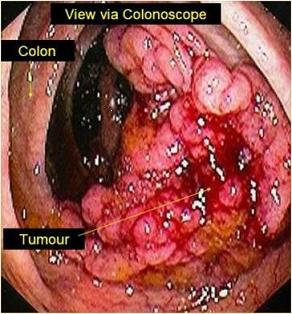 Symptomatic presentations often denote late stage disease. These symptoms include rectal bleeding, change in bowel habits, abdominal pain, decrease in stool caibre, passage of mucus, unexplained anaemia, bowel blockage, weight loss or loss of appetite.
Symptomatic presentations often denote late stage disease. These symptoms include rectal bleeding, change in bowel habits, abdominal pain, decrease in stool caibre, passage of mucus, unexplained anaemia, bowel blockage, weight loss or loss of appetite.
The early stage cancers are mostly diagnosed from screening procedures when patients are asymptomatic and this has contributed to better survival rates in colorectal cancers.
For the last two decades, prophylactic removal of colon polyps has been the standard approach to cancer prevention. Aggressive screening and polyps removal through colonscopy can reduce the rate of colon cancer development by approximately 80 percent.
Screening methods
Faecal Occult Blood Testing (FOBT)
Colorectal cancer bleeding may not be obvious to the naked eyes especially in the early stages. The advantage of this test is to pick up early stage cancers before patient presents with symptoms. It is also noninvasive and inexpensive.
Colonoscopy
Generally considered the gold standard for diagnosing colorectal cancer, colonoscopy has the main advantage of allowing diagnosis and definitive treatment of polyps.
Virtual Colonoscopy
Formidable developments in rendering 3-dimensional images using computer graphics have produced the technology of ‘virtual colonoscopy’. First described by Vining et al in 1994, virtual colonoscopy applies techniques for rendering complex images to spiral CT scan images. The computer then generates a retrograde intraluminal “fly through” navigation from rectum to caecum and repeats it in the opposite direction, allowing a detailed 3-dimensional view of the colonic lumen similar to real colonoscopy.
STAGING
Investigations for Staging
Once a colon or rectal cancer has been detected, preoperative staging, assessment of resectability, and assessment of the patient’s operative risks are indicated. The entire colon and rectum should be evaluated, usually with colonoscopy. Preoperative staging is done with CT scan abdomen and pelvis and chest Xrays or CT scan of lungs. Preoperative CEA, a cancer marker that can be detected in the blood, will provide an effective marker to monitor post- treatment disease recurrence in CEA-elevated patients.
ADVANCES IN TREATMENT
The management of colorectal cancers involves a multidisciplinary approach. This includes surgery, chemotherapy and radiotherapy. However, recent advances in surgical techniques and chemo-radiotherapy have resulted in lower morbidity and better clinical outcomes.
Surgery
Early stages of colorectal cancers are amenable to curative resections. Minimally invasive colorectal surgery for both benign and malignant conditions is available at Nobel Surgery Centre. Laparoscopic cancer surgery is safe, even for the elderly, and that the rates for tumour recurrence and patient survival are similar to open surgery. Laparoscopic colorectal surgery is advantageous over open surgery because it allows for smaller surgical wounds; leading to reduced post-operative pain, faster post-surgical recovery and earlier hospital discharge. Better surgical techniques, advanced surgical instrumentation and the availability of effective chemotherapy nowadays enable surgeons to resect low lying rectal tumours (1 – 2 cm above anal sphincter) without compromising anal function, thereby minimising the need for permanent stoma.
Chemo-radiation Therapy
Post-operative chemotherapy, with or without radiation therapy, is generally reserved for late stage colorectal cancer patients after surgical resection. However, a new concept of using ‘neo-adjuvant’ chemoradiation therapy, that is delivering combined radiotherapy and chemotherapy before surgery, is particularly useful for bulky, mid- to low-lying rectal cancers as a means of shrinking the tumour prior to surgical resection. This way, resection can be less radical and provides a better chance for preserving anal function and reducing recurrence rate.
CaseMdm L.S.L , 60years old female
|
PROGNOSIS
The 5 year survival rate for stage I is 90 percent and for stage II it is 75 percent. By the time rectal bleeding or change in bowel habits occur, the disease is likely to be at least stage III, which has a survival rate of around 70 percent. However, in stage IV disease, the 5 year survival significantly reduced to less than 30 percent.
Expert Author:
Dr Chen Chung Ming, Affinity Surgery Centre
The article above is meant to provide general information and does not replace a doctor's consultation.
Please see your doctor for professional advice.
